The corneal flap created during LASIK is one of the most elegant aspects of the procedure — and one of the most anxiety-inducing for patients. It’s a thin, living tissue hinge that gets lifted, repositioned, and then left to heal on its own without a single stitch. Understanding exactly how that flap heals, what’s happening at each stage, and what you should (and shouldn’t) be doing during recovery is the single most useful thing you can learn before or after your surgery.
This guide walks through each phase of LASIK flap healing — from the first hours when the flap is at its most vulnerable to the point months later when it’s fully integrated into the cornea. Whether you’re one day post-op and wondering if what you’re feeling is normal, or you’re researching LASIK and want to know what recovery actually looks like, this timeline will give you the clarity you need.
Key Takeaways
- The LASIK flap begins adhering to the cornea within minutes of repositioning — no stitches required.
- The first 24–48 hours are the most critical; the flap is fragile and can be displaced by rubbing or pressure.
- Most patients see significant visual improvement within the first week, but full flap stabilisation takes 1–3 months.
- Corneal nerve regeneration — which resolves dry eye — can take 3–6 months or longer.
Stage 1: Immediate Post-Op (First 24–48 Hours)
What’s Happening Inside Your Eye
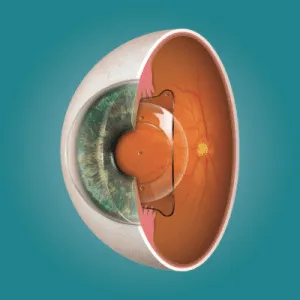
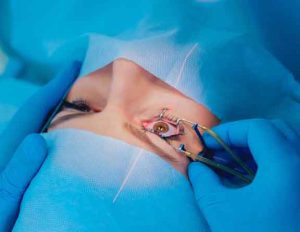
The moment your surgeon repositions the corneal flap after the excimer laser has reshaped the underlying stroma, the flap begins bonding to the tissue beneath it. This happens through a combination of natural surface tension and the dehydration pump of the corneal endothelium — essentially, the cornea pulls the flap down and holds it in place. Within minutes, the epithelial seal starts forming at the flap edge, and within hours, this seal is already providing preliminary adhesion.
During this window, your vision will be hazy or blurry — like looking through a fogged-up window. You’ll likely experience tearing, mild stinging or burning, light sensitivity, and a gritty sensation similar to having something in your eye. All of this is completely normal. The scratchiness typically peaks around 4–6 hours post-surgery and then gradually subsides.
What You Should Do
Sleep is the best thing you can do in the first few hours — your surgeon will likely encourage a long nap immediately after the procedure. Wear the protective eye shields provided, even during sleep, to prevent any accidental rubbing. Use your prescribed antibiotic and anti-inflammatory drops exactly on schedule, and apply preservative-free lubricating drops liberally. Most importantly: do not touch, rub, or press on your eyes for any reason.
Stage 2: Early Healing (Days 2–7)
What’s Happening Inside Your Eye
The epithelial cells are now actively migrating across the flap edge, creating a biological seal that progressively anchors the flap. By day 3 to 4, this epithelial bridge is well established, and the risk of accidental flap displacement drops significantly — though it hasn’t disappeared entirely. Your vision will improve noticeably during this period, and many patients are already seeing well enough to return to work and daily activities within 2–3 days.
Dryness, mild light sensitivity, and occasional fluctuations in visual clarity are still normal at this stage. You may notice halos or starbursts around lights at night — this is due to corneal swelling and will diminish as healing progresses.
What You Should Do
Continue all prescribed medications without exception. Keep wearing your eye shields at night for the full first week. Avoid getting water directly in your eyes during showers, stay away from dusty or smoky environments, and skip eye makeup entirely. This is also too early for swimming, hot tubs, or strenuous exercise — anything that increases eye pressure or introduces contaminants is off-limits.
Stage 3: Intermediate Recovery (Weeks 1–4)
What’s Happening Inside Your Eye
The flap is now well-seated and the epithelial seal is essentially complete. Beneath the surface, the stromal tissue at the interface between the flap and the bed is beginning to remodel — laying down new collagen fibres that will eventually provide structural strength. However, this stromal remodelling is slow and incomplete compared to pre-surgical tissue, which is why the flap interface never returns to its original tensile strength.
Vision is typically stable and clear by this point. Dry eye symptoms may persist because the corneal nerves severed during flap creation are still regenerating — these nerves are what trigger the reflex tear response, so their temporary absence means the eye doesn’t always “know” it needs lubrication.
What You Should Do
Most restrictions lift during this period. Your surgeon will likely clear you for light exercise, gentle eye makeup use, and a return to most normal activities. Continue lubricating drops as directed — even if your eyes feel fine, the tear film is still recovering. Avoid rubbing your eyes for at least another few weeks, and wear sunglasses outdoors to protect against UV exposure and wind-induced dryness.
Stage 4: Mature Healing (Months 1–3)
What’s Happening Inside Your Eye
The flap edges are now fully bonded to the surrounding corneal tissue. Stromal healing continues at the interface, and the flap achieves what clinicians consider long-term positional stability. For the vast majority of patients, the risk of flap dislocation from normal activities is now essentially zero. Vision reaches its optimal level during this phase — most patients achieve 6/6 (20/20) or better — and any residual visual artefacts like mild ghosting or glare have typically resolved.
If there’s a residual refractive error at the 3-month mark that hasn’t stabilised on its own, this is when your surgeon may discuss whether a LASIK enhancement is warranted.
What You Should Do
Attend your scheduled follow-up appointments — the assessments at 1 and 3 months are critical for confirming that your cornea has healed properly, your prescription is stable, and there are no subclinical issues like flap striae or early signs of ectasia. Maintain eye hydration habits, wear UV-protective sunglasses, and continue eating a nutrient-rich diet that supports corneal health — omega-3 fatty acids in particular support tear film quality.
Stage 5: Full Recovery (3–6 Months and Beyond)
What’s Happening Inside Your Eye
Corneal nerve regeneration, which began weeks ago, is now approaching completion. For most patients, this is when the last traces of dry eye resolve. The flap is fully integrated, and the cornea has reached its stable post-operative state. While the flap interface technically remains weaker than virgin corneal tissue indefinitely, this difference is clinically irrelevant for normal life — including contact sports, swimming, and vigorous physical activity.
What You Should Do
By this stage, all restrictions are lifted. Continue with annual eye examinations to monitor long-term corneal health and watch for age-related changes like presbyopia, which LASIK does not prevent. If you experience any sudden changes in vision quality years after surgery, see your eye care provider promptly — while late complications are rare, conditions like post-LASIK ectasia are treatable when caught early.
Factors That Affect How Your Flap Heals
Not everyone heals at exactly the same rate. Several variables influence your personal timeline. Patients with pre-existing dry eye tend to have a longer recovery period for tear film normalisation. The thickness of the flap created during surgery matters — thinner flaps created by femtosecond lasers tend to heal with better biomechanical stability than thicker microkeratome flaps. Age plays a role too: younger patients generally heal faster, but their prescriptions must be stable before surgery to prevent regression. Strict adherence to your post-operative drop schedule and activity restrictions makes a measurable difference in outcomes — patients who follow instructions consistently have fewer complications and faster visual recovery.
Warning Signs That Something Isn’t Right
While LASIK healing is overwhelmingly smooth, you should contact your surgeon immediately if you notice a sudden, significant drop in vision that wasn’t there the day before, increasing pain rather than decreasing pain after the first 24 hours, new redness or swelling that appears days after surgery, white or hazy patches visible in the cornea, or any discharge beyond normal tearing. These could indicate infection, inflammation (diffuse lamellar keratitis), or a flap irregularity — all of which are treatable when addressed promptly.
Conclusion
The LASIK flap healing process follows a predictable arc: fragile adhesion in the first hours, epithelial sealing in the first week, progressive stabilisation over the first month, and full structural integration by three to six months. Each stage comes with specific expectations and specific responsibilities — knowing what’s normal and what warrants a call to your surgeon removes the guesswork from recovery. The cornea is remarkably good at healing itself; your job is simply to stay out of its way while it does. If you’re planning LASIK and want a detailed, personalised recovery plan based on your corneal thickness, prescription, and lifestyle, book a consultation at Visual Aids Centre and our team will prepare you for every stage.
Frequently Asked Questions (FAQs)
Does the LASIK flap ever fully heal?
The flap bonds securely to the underlying cornea and achieves long-term stability, but the stromal interface never regains the full tensile strength of uncut tissue. For all practical purposes, the flap is permanent and stable after 3 months.
How long is the flap vulnerable to displacement?
The highest risk is in the first 24–48 hours. By one week, the epithelial seal provides significant protection. After one month, flap displacement from normal activities is extremely rare.
When can I rub my eyes after LASIK?
Most surgeons recommend avoiding eye rubbing for at least 2–4 weeks. Many advise making it a permanent habit to avoid rubbing, as it can contribute to other corneal conditions regardless of LASIK history.
Is it normal for vision to fluctuate during healing?
Yes. Mild visual fluctuations are common during the first 1–2 weeks as the cornea adjusts and the tear film stabilises. Persistent fluctuations beyond one month should be evaluated by your surgeon.
Can the flap be dislodged years after LASIK?
It’s extremely rare but technically possible with severe direct trauma to the eye. Normal activities including sports pose no meaningful risk after full healing.
How do I know if my flap has moved?
A displaced flap typically causes sudden blurring, pain, increased tearing, and light sensitivity. If you suspect displacement, contact your surgeon immediately — re-positioning is straightforward when done promptly.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Corneal Healing Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With more than four decades of clinical experience and over 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey has observed and managed the full spectrum of LASIK flap healing — from routine recoveries to the rare cases that require intervention. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey’s post-operative protocols at the centre are informed by hundreds of thousands of real patient outcomes. Learn more about our story and the clinical team behind Visual Aids Centre.