Three weeks after LASIK, most patients expect to be enjoying clear, comfortable vision — so when eye pain shows up at this stage, it is understandably alarming. The good news is that mild discomfort at the three-week mark is more common than many people realise, and it is usually manageable. The not-so-good news: certain types of pain at this point do require prompt attention.
This guide explains the most likely reasons you might still be experiencing eye pain three weeks after LASIK, how to tell the difference between normal healing discomfort and something that needs your surgeon’s involvement, and what practical steps you can take right now to feel more comfortable. Understanding how LASIK works — and what it does to the cornea — makes it easier to understand why some discomfort at this stage is expected. The recovery principles below apply regardless of which procedure you had, and knowing the typical flap healing stages will help you gauge where you are in the process.
Key Takeaways
- Mild aching, foreign-body sensation, or intermittent stinging at 3 weeks is often related to dry eye or corneal nerve regeneration — both normal parts of healing.
- Sharp, stabbing, or worsening pain that does not respond to lubricating drops is not normal and warrants an urgent check-up.
- Dry eye syndrome is the single most common cause of post-LASIK discomfort at the 3-week stage.
- Redness, discharge, light sensitivity, or sudden vision changes alongside pain should be evaluated the same day.
Where You Are in the LASIK Healing Timeline
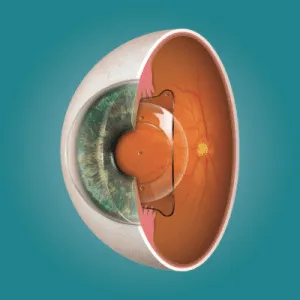
To understand why pain at three weeks is not automatically a red flag, it helps to know what is happening beneath the surface. During LASIK, a thin corneal flap is created and repositioned after the excimer laser reshapes the underlying stroma. The surface epithelium heals within the first 24–48 hours, but the deeper structures — the stromal bed, the flap interface, and especially the corneal nerves — take considerably longer.
Corneal nerves are severed during flap creation. These nerves are responsible for triggering tear production and for the protective blink reflex. Their regeneration begins within weeks but can take 3 to 6 months to complete — and during that window, the eye’s surface is vulnerable to dryness, sensitivity, and intermittent discomfort. At the three-week mark, you are in the middle of this nerve recovery phase, which is why some degree of ocular discomfort is clinically expected.
Common Causes of Eye Pain at 3 Weeks
Dry Eye Syndrome
This is by far the most frequent cause. With corneal nerves still regenerating, the feedback loop that tells your lacrimal glands to produce tears is compromised. The result is a dry, gritty, stinging, or burning sensation that can range from mild annoyance to genuine pain — especially during prolonged screen work, in air-conditioned rooms, or at the end of the day. If your eyes feel worse in the morning or after long reading sessions, dry eye is the likely culprit. For management strategies, our guide on treating dry eyes after LASIK offers detailed advice.
Corneal Nerve Regeneration
As severed nerve fibres regrow, they can sometimes produce unusual sensations — brief shooting pains, a prickling or tingling feeling, or transient aching that comes and goes without a clear trigger. This is sometimes called “neuropathic” discomfort and is a sign that healing is progressing, not stalling. It typically resolves on its own as the nerve network matures over the following months.
Residual Inflammation
Even though the visible healing looks complete by week three, low-grade inflammation at the flap interface can persist. This is one reason surgeons prescribe steroid or anti-inflammatory eye drops for several weeks after LASIK. If you have already finished your prescribed course, lingering inflammation may produce a dull ache or mild sensitivity. Your surgeon can check for signs of diffuse lamellar keratitis (DLK) — a condition where the flap interface develops inflammation that requires treatment.
Eye Strain from Returning to Screens Too Quickly
Many patients jump back into heavy screen use within the first week. By week three, the cumulative effect of insufficient blinking during screen time can contribute to discomfort that feels like deep eye pain. The 20-20-20 rule (every 20 minutes, look at something 20 feet away for 20 seconds) is particularly important during this period. For tips on managing screen-related strain, our article on reducing eye strain after LASIK covers practical strategies.
When Eye Pain Signals Something More Serious
While most three-week discomfort is benign, there are situations where pain indicates a problem that needs clinical intervention.
Infection
Post-LASIK infection is rare — but not impossible — at the three-week mark. Warning signs include increasing pain rather than decreasing, redness that is worsening instead of improving, discharge (especially if cloudy or yellowish), and light sensitivity. If you suspect infection, this is a same-day emergency. Early treatment with targeted antibiotics protects your visual outcome. For more on recognising these signs, see signs of eye infection after LASIK.
Flap Complications
Although uncommon, issues such as microscopic flap wrinkles (striae) or epithelial ingrowth beneath the flap can produce pain, blurred vision, or a foreign-body sensation weeks after surgery. These conditions are diagnosable at a slit-lamp examination and treatable if caught early.
Elevated Eye Pressure
Post-operative steroid eye drops — while essential for controlling inflammation — can cause a steroid-induced rise in intraocular pressure (IOP) in some patients. This can manifest as a deep aching sensation, headache behind the eye, or a feeling of pressure. If you are still using steroid drops at week three and experiencing these symptoms, your surgeon should check your intraocular pressure and adjust your medication accordingly.
What You Can Do at Home
Use preservative-free lubricating drops generously. At three weeks, most patients underestimate how often they need artificial tears. Apply them every 1–2 hours during screen work and at least 4–6 times per day otherwise. For guidance on choosing the right product, see our page on the best lubricating eye drops after LASIK.
Apply warm compresses. A clean, warm cloth held gently over closed eyelids for 5–10 minutes can stimulate the meibomian glands to release oils into the tear film, improving tear quality and reducing evaporative dryness. Our guide on warm compresses after LASIK explains the technique in detail.
Limit screen time and follow the 20-20-20 rule. Blinking rate drops by up to 60% during screen use. Conscious blinking and regular breaks make a measurable difference in comfort at this stage of recovery.
Avoid rubbing your eyes. The flap is still settling at three weeks. Rubbing can introduce bacteria, irritate the surface, and in extreme cases displace the flap. If you have an itch or foreign-body sensation, use lubricating drops instead of rubbing — for more on why this matters, see our article on rubbing eyes after LASIK.
Wear sunglasses outdoors. UV exposure and wind both worsen surface dryness and sensitivity. Wraparound-style sunglasses provide the best protection during the early months of recovery.
When to Contact Your Surgeon Immediately
Do not wait for your next scheduled follow-up if you experience any of the following: sharp or stabbing pain that is getting worse rather than better, sudden decrease in vision clarity, redness that is spreading or deepening in colour, any discharge from the eye, severe light sensitivity that prevents you from opening your eyes comfortably, or a persistent headache combined with eye pressure. These symptoms could indicate infection, flap displacement, DLK, or steroid-induced pressure elevation — all of which are treatable but time-sensitive. At Visual Aids Centre, our post-operative care team is available for urgent consultations precisely because we understand that recovery concerns do not always happen during business hours.
How to Support Healing and Prevent Prolonged Discomfort
Attend every follow-up appointment. Scheduled post-operative visits exist to catch subtle issues before they become symptomatic. Even if your vision feels fine, your surgeon can detect early signs of dry eye, inflammation, or pressure changes that you may not notice yet.
Complete your full medication course. Stopping steroid or antibiotic drops early — because you “feel fine” — is one of the most common reasons patients develop delayed complications. Use every drop as prescribed, for the full duration.
Stay hydrated and consider omega-3 supplementation. Systemic hydration supports tear production, and omega-3 fatty acids from fish oil or flaxseed have been shown to improve tear film quality during the post-LASIK dry eye phase.
Avoid environmental irritants. Smoke, dust, strong perfumes, and prolonged air conditioning exposure all worsen ocular surface discomfort during recovery. If you work in a dusty or air-conditioned environment, a desk humidifier can make a noticeable difference.
Conclusion
Eye pain three weeks after LASIK is, in most cases, a manageable symptom of the normal healing process — driven primarily by dry eye and corneal nerve regeneration. It does not mean something has gone wrong. However, it does deserve attention: mild discomfort should be improving (not worsening), and any pain accompanied by redness, discharge, vision changes, or light sensitivity needs prompt evaluation. The single most effective thing you can do right now is use preservative-free lubricating drops frequently, avoid rubbing, and attend your follow-up visits. If your pain is not improving or you are unsure whether what you are experiencing is normal, contact Visual Aids Centre — our team will assess your healing status and put your mind at ease.
Frequently Asked Questions (FAQs)
Is it normal to have eye pain 3 weeks after LASIK?
Mild discomfort — such as dryness, grittiness, or intermittent stinging — is common at three weeks and usually related to dry eye or nerve regeneration. Sharp or worsening pain is not normal and should be evaluated by your surgeon.
How long does post-LASIK eye pain typically last?
Most acute pain resolves within the first 24–48 hours. Mild dryness-related discomfort can persist for 1–3 months as corneal nerves regenerate. Significant pain beyond a few days post-surgery should always be checked.
Can dry eye cause real pain after LASIK, or just mild discomfort?
Dry eye can cause genuine pain, not just irritation. Severe dryness produces a burning, stinging, or aching sensation that some patients describe as moderate to significant pain — especially during screen use or in air-conditioned environments.
Should I stop using steroid drops if my eye hurts at 3 weeks?
Never stop or adjust prescribed eye drops without consulting your surgeon. Steroid drops control inflammation, but they can also raise eye pressure in some patients. Your surgeon needs to evaluate whether the drops should be continued, tapered, or switched.
When should I go to the emergency room for eye pain after LASIK?
Seek urgent care if you experience sudden severe pain, rapid vision loss, heavy discharge, or extreme light sensitivity. These could indicate infection or a flap complication that requires immediate treatment.
Can screen time make post-LASIK eye pain worse?
Yes. Screen use reduces your blink rate, which accelerates tear evaporation and worsens dryness-related pain. Following the 20-20-20 rule and using lubricating drops during screen work helps significantly.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Post-Operative Care Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With more than four decades of clinical experience and over 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey and the clinical team have managed thousands of post-operative recovery cases — from routine dry eye to complex flap complications. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey personally oversees the post-operative care protocols at Visual Aids Centre to ensure every patient’s recovery stays on track. Learn more about our achievements and legacy.