LASIK has helped millions of people shed their glasses permanently—but the procedure only delivers those results when the right patient is matched to it. That matching process is precisely why contraindications exist. A contraindication isn’t a bureaucratic hurdle; it’s a clinical signal that performing LASIK on a particular eye, at a particular time, would create more risk than benefit. Understanding what disqualifies someone—and why—is one of the most useful things any prospective patient can know before walking into a consultation.
This guide covers every major LASIK contraindication clearly and honestly: the anatomical factors, the systemic health conditions, the age considerations, and the lifestyle variables that surgeons weigh before recommending the procedure. If any of these apply to you, you’ll also find what the alternatives typically look like.
Key Takeaways
- LASIK is not suitable for patients under 18, or for older adults with presbyopia as their primary vision complaint.
- Thin or irregularly shaped corneas—particularly keratoconus—are among the most clinically significant contraindications.
- Active eye infections, severe dry eye, glaucoma, cataracts, and retinal disorders all preclude LASIK, either temporarily or permanently.
- Systemic conditions including uncontrolled diabetes, autoimmune disease, and pregnancy affect healing and may disqualify a patient.
- Patients who do not qualify for LASIK often have viable alternatives—PRK, EVO-ICL, Trans-PRK, or refractive lens exchange—worth exploring.
Age-Related Factors
Under 18: Eyes Still Developing
LASIK requires that the eye has finished its natural growth and refractive development. For most patients this happens in their late teens, which is why the minimum age threshold is 18 years. Operating before stabilisation is complete risks correcting a moving target—the prescription continues shifting post-surgery, delivering an outcome that was obsolete the moment it was made. Our guide on the best age for LASIK explains the developmental reasoning and what age-related milestones surgeons actually look for.
Over 40: Presbyopia Enters the Picture
LASIK corrects corneal refractive errors—myopia, hypermetropia, astigmatism—but it does not address presbyopia, the age-related stiffening of the crystalline lens that causes difficulty with near focus. Patients over 40 who are primarily troubled by reading difficulty may find that LASIK delivers excellent distance vision but still requires reading glasses. This isn’t a failure of the procedure; it’s a limitation that needs to be clearly understood upfront. Our article on correcting presbyopia after LASIK covers what options exist if this becomes a concern post-operatively.
Unstable or Fluctuating Prescription
LASIK produces lasting results when it corrects a stable, established prescription. If your spectacle power has changed by more than 0.5 dioptres in the past 12–24 months, your eyes are still shifting—and LASIK on a drifting prescription typically leads to either under-correction or a need for re-treatment within a few years. The most common causes of prescription instability include hormonal fluctuations, corticosteroid use, and ongoing unmanaged eye conditions. This is also why patients with prescriptions at the outer limits of the treatable range require particularly careful assessment before proceeding.
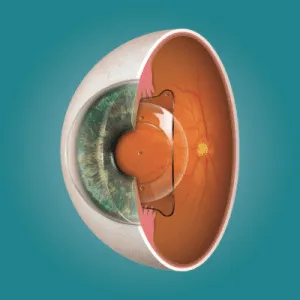
Corneal Thickness and Shape
Thin Corneas and Ectasia Risk
LASIK removes corneal tissue to reshape the optical surface. If the cornea is too thin to begin with, insufficient tissue remains after the procedure to maintain structural integrity—and the cornea can begin to bulge forward under normal intraocular pressure. This condition, called post-LASIK ectasia, is among the most serious complications associated with the procedure and is the primary reason corneal thickness assessment is mandatory before surgery.
Keratoconus and Irregular Corneas
Keratoconus—a progressive condition where the cornea thins and takes on a cone-like shape—is a firm contraindication for LASIK. The procedure would accelerate the structural weakening already underway, with potentially severe visual consequences. Even subclinical or suspected keratoconus, which may not yet cause noticeable symptoms, is sufficient reason to decline the procedure. Patients with keratoconus are typically candidates for corneal cross-linking (C3R) to arrest progression.
Current or Prior Eye Conditions
Dry Eye Syndrome
LASIK temporarily disrupts the corneal nerves that govern tear secretion, which is why mild dryness is a near-universal post-operative experience. In patients with pre-existing dry eye syndrome, this disruption is amplified—sometimes severely—leading to chronic discomfort, fluctuating vision, and impaired healing. Moderate to severe dry eye is typically a contraindication until the condition is adequately managed. Our article on LASIK in the context of keratoconjunctivitis sicca addresses this specific diagnostic category directly.
Glaucoma
The corneal reshaping performed during LASIK alters the physical properties of the cornea in ways that affect intraocular pressure (IOP) readings. Since IOP measurement is the primary tool for managing glaucoma, LASIK makes it significantly harder to monitor the condition accurately after surgery. For patients with advanced or poorly controlled glaucoma, this interference is clinically unacceptable.
Retinal Disorders
Conditions including retinal detachment, diabetic retinopathy, and retinal holes all represent contraindications—either absolute or relative depending on severity. LASIK addresses the cornea, not the retina, so it cannot help these patients visually, and the procedure itself carries added risk in eyes with compromised retinal health. If you have been told you have retinal pathology, our article on whether LASIK is possible with retinal holes explains how individual assessment works in these cases.
Active Infections and Cataracts
Any active ocular infection—bacterial, viral, or fungal—must be fully resolved before LASIK is considered. Operating on an infected eye dramatically increases the risk of spreading the infection into the surgical site. Similarly, cataracts that are already impairing vision are better addressed through cataract surgery, which can incorporate refractive correction simultaneously, rather than adding LASIK on top of an already compromised lens.
Systemic and Autoimmune Diseases
Uncontrolled Diabetes
Poorly controlled diabetes impairs wound healing across all tissues—the cornea is no exception. Fluctuating blood glucose also causes fluctuating lens refraction, making it difficult to establish a stable pre-operative prescription. Well-controlled diabetics may still be candidates, assessed individually.
Autoimmune Conditions: Lupus, Rheumatoid Arthritis, Hashimoto’s
Autoimmune diseases create unpredictable healing environments. Corneal wounds that would resolve cleanly in a healthy immune system may heal slowly, irregularly, or with scarring in patients whose immune response is dysregulated. Patients taking immunosuppressive medications face compounded infection risk. This applies to a wide range of autoimmune diagnoses. Our articles on LASIK for lupus patients and LASIK with Hashimoto’s disease go into the condition-specific nuances that determine whether a patient can safely proceed.
Pregnancy and Breastfeeding
Hormonal changes during pregnancy and lactation cause temporary fluctuations in corneal curvature and refractive error—meaning the prescription measured during these periods may not represent the eye’s stable baseline. Additionally, several medications standard in the LASIK post-operative protocol (antibiotics, anti-inflammatories) carry restrictions during pregnancy and breastfeeding. Most surgeons advise waiting at least three to six months after weaning before undergoing LASIK, once prescription stability is confirmed.
Lifestyle and Occupational Factors
Certain professions and activities introduce a contraindication that is less clinical and more situational. Professional athletes in high-impact or contact sports—boxing, martial arts, rugby—face an elevated risk of post-operative flap trauma that makes flapless procedures a better fit. Military personnel and some government service roles are subject to institutional guidelines about LASIK that vary by organisation and should be confirmed with the relevant authority before proceeding.
Psychological readiness is also a genuine consideration. LASIK requires a cooperative patient during a procedure that, though brief, involves lying still with the eye held open by a speculum. Patients with severe procedural anxiety or certain untreated mental health conditions that affect compliance with post-operative care may require additional preparation before the procedure is appropriate.
Other Considerations
Patients who have already had a refractive procedure—whether a prior LASIK, PRK, or other corneal surgery—may still be candidates for enhancement, but only if residual corneal thickness is adequate and the overall ocular profile supports it. This requires an individual assessment rather than a blanket answer. Our guide on having LASIK more than once explains the eligibility criteria and what surgeons look for in repeat-procedure candidates.
If You Don’t Qualify: What Are the Alternatives?
A LASIK contraindication is not the end of the road for vision correction—it is a redirect toward the procedure that is actually appropriate for your eyes. The most commonly recommended alternatives include:
- Trans-PRK / Surface Ablation — suitable for patients with thinner corneas who are not keratoconus-positive; no flap is created, reducing structural risk.
- EVO-ICL — an implantable collamer lens placed inside the eye without removing corneal tissue; well-suited for patients with thin corneas or very high prescriptions.
- Refractive Lens Exchange (RLE) — replacing the natural lens with a premium intraocular lens; particularly relevant for patients over 45 where presbyopia is a significant component.
- C3R (Corneal Cross-Linking) — for keratoconus patients, C3R arrests progression rather than correcting the refractive error, but it is often the safest first intervention before any vision correction is considered.
Conclusion
LASIK contraindications exist to protect patients, not to exclude them arbitrarily. Every item on this list—from corneal thickness to autoimmune disease to age—reflects a genuine clinical reason why the procedure would carry elevated risk or deliver compromised outcomes for a specific individual. The right response to a contraindication is not frustration; it’s a conversation with an experienced surgeon about which alternative best matches your eyes, your health, and your goals.
At Visual Aids Centre, every LASIK consultation begins with a thorough pre-operative assessment that covers corneal topography, tear film analysis, prescription stability, and a complete medical history—precisely because matching the right procedure to the right patient is what produces results that last. If you want a clear, honest picture of your eligibility, book a consultation with our team.
Frequently Asked Questions (FAQs)
Can I get LASIK if I have dry eyes?
Mild dry eye does not automatically disqualify you, but moderate to severe dry eye syndrome is a significant contraindication. Most surgeons require the condition to be adequately managed—with artificial tears, punctal plugs, or other treatments—before LASIK is considered.
Can patients with keratoconus get LASIK?
No. Keratoconus is a firm contraindication for LASIK—the procedure would accelerate corneal thinning and potentially cause serious complications. Patients with keratoconus are typically assessed for corneal cross-linking (C3R) to stabilise the condition, after which other visual correction options may be explored.
Is LASIK safe for diabetic patients?
It depends on how well-controlled the diabetes is. Uncontrolled diabetes impairs corneal healing and causes prescription instability through lens changes. Well-controlled diabetics may still qualify after thorough individual assessment. See our dedicated guide on LASIK for patients with type 2 diabetes for the clinical criteria involved.
Can autoimmune disease rule out LASIK?
Conditions like lupus, rheumatoid arthritis, and Hashimoto’s thyroiditis can all affect healing and infection risk after LASIK, making them relative or absolute contraindications depending on disease activity and medication status. Individual assessment by an experienced surgeon is required.
What are the alternatives if I don’t qualify for LASIK?
The most common alternatives include Trans-PRK (for thinner corneas), EVO-ICL (for patients unsuitable for corneal procedures), Refractive Lens Exchange (for patients over 45 with presbyopia), and C3R for keratoconus stabilisation.
Can I get LASIK after a previous refractive surgery?
Possibly, but only if residual corneal thickness is sufficient and the overall ocular profile supports it.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Post-Operative Care Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With more than four decades of clinical experience and over 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey has developed the pre-operative assessment protocols that determine LASIK eligibility at the centre—including the clinical criteria for contraindication, alternative procedure selection, and the management of complex cases involving systemic disease or corneal pathology. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey personally reviews all clinical content at Visual Aids Centre to ensure it reflects current evidence and serves genuine patient need. Learn more about the centre’s clinical philosophy and history at our story.