By three months after LASIK, the vast majority of patients are enjoying clear, comfortable vision with no lingering discomfort. So if your eyes still hurt at this stage, it’s understandable to feel concerned. The reassuring news: persistent eye pain at three months is uncommon, but when it does occur, it almost always points to a specific, treatable cause — not a sign that the surgery has gone fundamentally wrong.
The most important thing you can do is not ignore it. Pain that persists well past the normal healing window deserves a thorough evaluation, not just reassurance that “it takes time.” This guide walks through the most common reasons for eye pain three months after LASIK, explains what each one feels like so you can describe your symptoms accurately to your surgeon, and outlines the treatment options that resolve each cause. Whether the pain is a dull ache, a sharp sting, or a burning sensation, understanding what’s driving it is the first step toward getting it resolved.
Key Takeaways
- Eye pain persisting at 3 months is not part of normal LASIK recovery — it signals an underlying issue that needs evaluation.
- Chronic dry eye is the most common cause by far, followed by corneal neuropathy (nerve healing irregularities).
- Less common but important causes include epithelial ingrowth, residual refractive error causing strain, and meibomian gland dysfunction.
- Nearly all causes of late post-LASIK pain are treatable once correctly diagnosed.
What Does Normal LASIK Recovery Look Like?
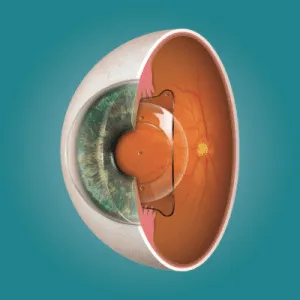
Understanding the typical healing timeline helps put late-onset pain in perspective. In the first 24–48 hours after LASIK, mild soreness, tearing, and light sensitivity are expected. By one week, the corneal flap has re-adhered and surface discomfort has largely resolved. Between weeks 2 and 6, some patients experience fluctuating dryness and occasional mild strain — particularly during prolonged screen use — as the corneal nerves begin regenerating. By month 3, the corneal surface should be stable, the tear film should be functional, and any procedural discomfort should be completely gone.
If you’re still experiencing genuine pain — not the brief, occasional dryness that a drop of artificial tears resolves — at the three-month mark, that’s outside the expected recovery window and warrants investigation.
Why Your Eyes Still Hurt at 3 Months
Chronic Dry Eye Syndrome
This is the single most common explanation for persistent discomfort after LASIK, accounting for the majority of late pain complaints. During the procedure, corneal nerves that regulate tear production are severed. In most patients, these nerves regenerate within 3–6 months and tear function returns to normal. But in a subset of patients — particularly those with pre-existing borderline dry eye, contact lens overuse, or autoimmune conditions — the nerve recovery is slower or incomplete, leaving the ocular surface chronically under-lubricated.
Dry-eye-related pain typically presents as a gritty, sandy, or burning sensation that worsens with screen time, air conditioning, or wind exposure. It may improve temporarily with lubricating drops but return within minutes. If standard artificial tears aren’t providing adequate relief, prescription options like cyclosporine drops or LipiFlow treatment for meibomian gland dysfunction can address the root cause rather than just the symptoms. For a deeper look at why dryness persists long-term, see our guide on permanent dry eyes after LASIK.
Corneal Neuropathy (Nerve Healing Irregularities)
When the severed corneal nerves regenerate after LASIK, they occasionally reconnect in abnormal patterns — a condition known as corneal neuralgia or neuropathic pain. This creates a disconnect between the physical state of the eye (which may look perfectly healthy on examination) and what the patient feels (which can include burning, stabbing, aching, or a constant feeling of pressure). It’s one of the most frustrating post-LASIK conditions because the eye appears normal, yet the pain is very real.
Corneal neuropathy is more common after high-correction procedures and in patients with a history of migraines or chronic pain conditions. Treatment typically involves medications that target nerve pain — such as low-dose gabapentin or amitriptyline — rather than standard eye drops. For more on how nerve damage presents after LASIK, read about symptoms of nerve damage after LASIK.
Meibomian Gland Dysfunction (MGD)
The meibomian glands in your eyelids produce the oily layer that prevents tears from evaporating too quickly. LASIK can disrupt the function of these glands, leading to a condition called evaporative dry eye — where your eyes produce enough tears, but the tears evaporate before they can do their job. The result is a burning, irritated feeling that conventional artificial tears may not fully address because the problem isn’t tear volume but tear quality.
MGD responds well to warm compresses applied to the closed eyelids for 10 minutes daily, gentle lid massage, and in stubborn cases, professional in-office treatments that clear blocked glands. Your surgeon can diagnose MGD with a simple examination of the eyelid margins.
Epithelial Ingrowth or Flap Complications
In rare cases, cells from the corneal surface can migrate underneath the flap — a condition called epithelial ingrowth. Small amounts may cause no symptoms, but larger ingrowths can produce a foreign-body sensation, intermittent sharp pain, and blurred vision. Flap-related issues such as microscopic wrinkles (striae) can also cause persistent discomfort, light sensitivity, or ghosting that patients describe as pain.
Both conditions are identifiable through a detailed slit-lamp examination and corneal imaging. If confirmed, your surgeon can lift the flap, remove the ingrown cells, and smooth any irregularities — typically resolving the pain completely.
Residual Refractive Error Causing Eye Strain
If LASIK didn’t fully correct your prescription — or if a small degree of regression has occurred — your eyes may be working harder than they should to focus, especially during close work. This sustained effort produces eye strain that manifests as aching behind the eyes, forehead tension, and fatigue that builds throughout the day. Patients often describe this as pain, though it’s mechanically closer to muscular fatigue.
A refraction test at your follow-up appointment will reveal whether a residual prescription exists. If it does, options include an enhancement procedure, prescription glasses for specific tasks, or simply confirming that the remaining error is too small to require intervention and will stabilise on its own.
Environmental and Lifestyle Factors
It’s worth considering whether external factors are aggravating your healing eyes. Prolonged computer use significantly reduces blink rate, air conditioning and heating dry the ocular surface, and Delhi’s air quality during winter months can introduce irritants that a fully healed eye tolerates but a still-recovering eye may not. These factors don’t cause the underlying problem, but they can amplify discomfort from any of the conditions listed above.
When to Contact Your Surgeon
Any eye pain at three months post-LASIK warrants a clinical evaluation, but certain patterns require more urgent attention. Seek a same-day or next-day appointment if the pain is sudden and severe (rather than the gradual, chronic discomfort of dry eye), if it’s accompanied by a noticeable drop in vision clarity, if you see increasing redness or inflammation that isn’t responding to lubricating drops, if you experience discharge from the eye, or if the pain is only in one eye and worsening — this pattern can indicate a flap complication or localised infection that needs prompt treatment. Don’t assume late-onset pain is “just dryness” — the only way to know for certain is a thorough examination with corneal imaging.
How Late Post-LASIK Pain Is Treated
Treatment depends entirely on the diagnosis. For chronic dry eye, the approach escalates from preservative-free artificial tears to prescription anti-inflammatory drops (like cyclosporine), punctal plugs to retain your natural tears, omega-3 supplementation, and in-office meibomian gland treatments. For corneal neuropathy, low-dose nerve-modulating medications, autologous serum eye drops, or scleral contact lenses that bathe the corneal surface in a constant layer of fluid can provide significant relief. Epithelial ingrowth or flap irregularities typically require a minor surgical procedure to lift the flap and correct the issue. Residual refractive errors may be addressed with an enhancement procedure or corrective lenses depending on your corneal thickness and the degree of remaining error.
The key point: none of these conditions require you to simply live with the pain. Each has a defined treatment pathway, and most patients experience substantial improvement once the correct diagnosis is made.
What You Can Do at Home
While waiting for your evaluation, several measures can reduce discomfort. Use preservative-free artificial tears frequently — every 1–2 hours if needed. Apply warm compresses to your closed eyelids for 10 minutes morning and evening to support meibomian gland function. Follow the 20-20-20 rule during screen work (every 20 minutes, look at something 20 feet away for 20 seconds). Wear wrap-around sunglasses outdoors to protect against wind and UV exposure. Stay well hydrated, and consider adding omega-3 fatty acids to your diet through fish, flaxseed, or supplements — there’s solid evidence that omega-3s support tear film quality. Avoid rubbing your eyes, even if they feel itchy — mechanical pressure on a healing cornea can worsen both dry eye and any underlying flap issues.
Conclusion
Eye pain three months after LASIK falls outside the normal recovery window and always deserves clinical attention — but it’s rarely a sign of something irreversible. The most common cause is chronic dry eye, followed by corneal nerve healing irregularities, and both respond well to targeted treatment. Less common causes like epithelial ingrowth, flap complications, and residual refractive error are identifiable through standard diagnostic tests and treatable in the vast majority of cases. The most important step is getting evaluated rather than waiting and hoping the pain resolves on its own. If you’re experiencing persistent discomfort after LASIK, book a consultation at Visual Aids Centre — our team will identify the cause and build a treatment plan to resolve it.
Frequently Asked Questions (FAQs)
Is eye pain 3 months after LASIK normal?
No. By three months, procedural discomfort should be fully resolved. Persistent pain indicates an underlying condition — most commonly chronic dry eye or corneal neuropathy — that needs evaluation and treatment.
What does corneal neuropathy feel like after LASIK?
Burning, stabbing, or a constant aching pressure behind the eye, often with an eye that appears completely normal on surface examination. It’s caused by irregular nerve regeneration and responds to nerve-modulating medications.
Can dry eye cause actual pain months after LASIK?
Yes. Chronic dryness causes the corneal surface to become rough and inflamed, producing a gritty, burning sensation that can be genuinely painful — especially during screen use, in air-conditioned environments, or on windy days.
Will the pain go away on its own?
Some cases of late dry eye do gradually improve as corneal nerves continue regenerating over 6–12 months. However, neuropathic pain, epithelial ingrowth, and flap complications rarely self-resolve and need active treatment.
Should I see the surgeon who performed my LASIK or a different specialist?
Start with your original surgeon — they have your pre-operative data and surgical records. If the cause isn’t identified or treatment isn’t resolving the issue, a corneal specialist or dry eye specialist can provide a second opinion.
Can the pain be a sign of a serious complication like ectasia?
It’s possible but rare. Post-LASIK ectasia typically presents as progressive blurring and distorted vision rather than pain alone. Your surgeon can rule it out with corneal topography and thickness measurements at your follow-up.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Post-Operative Care Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With more than four decades of clinical experience and over 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey has managed the full spectrum of post-LASIK complications — from routine dry eye to complex cases of corneal neuropathy and flap-related issues. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey’s approach to persistent post-operative pain is informed by real outcome data from hundreds of thousands of cases. Learn more about our story.