LASIK has helped millions of people ditch their glasses—but like any surgical procedure, it comes with risks worth understanding. One of the rarest yet most anxiety-inducing complications is LASIK flap dislocation, where the thin corneal flap created during surgery shifts out of position. The good news? It is uncommon, highly treatable when caught early, and largely preventable with proper post-operative care.
Whether you are considering LASIK, recovering from the procedure, or simply researching potential complications, this guide gives you a clear, practical understanding of what flap dislocation actually involves—why it happens, how to recognise it, and what to do if it occurs. At Visual Aids Centre, our team has managed over 250,000 laser vision correction procedures, and flap-related complications are something we take seriously from the very first consultation.
Key Takeaways
- LASIK flap dislocation is rare but can occur in the early healing phase or, very occasionally, years later following eye trauma.
- Symptoms include sudden blurry vision, pain, light sensitivity, and a foreign-body sensation—seek immediate care if these appear.
- Treatment involves prompt surgical repositioning of the flap, and outcomes are excellent when addressed quickly.
- Prevention centres on avoiding eye rubbing, wearing protective eyewear, and attending all follow-up appointments.
What Is LASIK Flap Dislocation?
Understanding the LASIK Flap
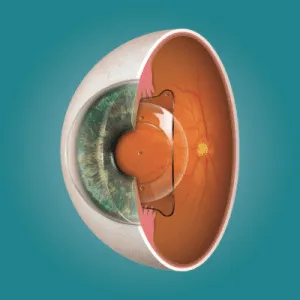
During LASIK surgery, a specialised femtosecond laser creates a thin, hinged flap on the surface of the cornea. This flap is gently lifted so that an excimer laser can reshape the underlying corneal tissue—correcting refractive errors such as myopia, hyperopia, and astigmatism. Once the reshaping is complete, the flap is repositioned onto the cornea, where it adheres naturally without stitches. Over the following days and weeks, the epithelium seals the flap edges and the tissue bond strengthens progressively.
How Does Flap Dislocation Occur?
Dislocation happens when the flap moves from its intended position, partially or completely losing contact with the underlying stroma. A partial dislocation means only a section of the flap has lifted, while a complete dislocation involves the entire flap becoming detached. Either scenario disrupts the smooth optical surface of the cornea, leading to immediate vision problems and discomfort.
The risk is highest during the initial healing phase—typically the first 24 to 72 hours—when the flap–stroma bond is still forming. However, because the LASIK flap never fully fuses with the same strength as undisturbed tissue, trauma to the eye can theoretically displace it even months or years later, though this is exceedingly uncommon.
Causes of Flap Dislocation
Several factors can increase the likelihood of flap displacement after LASIK. Understanding them helps you take the right precautions during recovery and beyond.
Eye Rubbing
This is the single most common preventable cause. Vigorous rubbing—especially in the first few weeks—can mechanically shift the flap before it has fully adhered. Even at the six-month mark, rubbing remains inadvisable because the flap interface never regains the tensile strength of virgin corneal tissue.
Blunt Trauma or Injury
A direct blow to the eye—from a ball, an elbow during sports, or even an accidental poke—can displace the flap weeks, months, or in rare cases years after LASIK. This is why athletes considering LASIK should discuss flapless alternatives like SMILE Pro with their surgeon.
Chronic Dry Eye
Prolonged dry eye conditions can weaken the adhesion between the flap and the stroma. A healthy tear film plays a critical role in corneal surface healing, and compromised lubrication can leave the flap more vulnerable to displacement.
Incomplete Adhesion or Healing
In a small number of patients, the flap may not bond as expected during the initial healing window. Pre-existing corneal irregularities, unusually thin corneas, or conditions like diffuse lamellar keratitis (DLK) can interfere with normal flap adhesion.
High-Impact Activities Without Protection
Contact sports, adventure activities, or any scenario where the eyes are exposed to impact without protective eyewear can pose a significant risk—even years after surgery.
Symptoms of a Dislocated Flap
Recognising the warning signs early is crucial. If you experience any of the following after LASIK—whether days or years post-surgery—contact your eye care provider immediately:
- Sudden blurred or distorted vision that does not improve with blinking.
- Sharp or unusual eye pain that feels different from normal post-operative soreness.
- Foreign body sensation—a persistent feeling that something is in your eye.
- Excessive tearing and redness beyond what is typical during recovery.
- Increased light sensitivity that appears suddenly or worsens without explanation.
These symptoms can overlap with other post-LASIK issues such as infection or epithelial ingrowth, which is precisely why a professional evaluation—not self-diagnosis—is essential. At Visual Aids Centre, we prioritise same-day emergency assessments for any patient reporting acute symptoms after laser vision correction.
Treatment and Recovery
The standard treatment for a dislocated LASIK flap is a procedure called flap repositioning. Here is what the process typically involves:
- Immediate consultation. The ophthalmologist examines the eye under a slit lamp to assess the degree of displacement and check for debris or folds beneath the flap.
- Flap lift and repositioning. Under local anaesthetic drops, the surgeon gently lifts the displaced flap, irrigates the interface to remove any trapped particles, and carefully repositions the flap to its correct alignment.
- Smoothing and inspection. The flap is smoothed out meticulously to eliminate wrinkles or striae that could cause irregular astigmatism.
- Bandage contact lens. A therapeutic contact lens may be placed over the cornea to stabilise the flap and improve comfort during healing.
- Post-operative medication. Antibiotic and anti-inflammatory drops are prescribed to prevent infection and manage swelling. Your surgeon will outline the exact drop schedule for your situation.
- Close follow-up monitoring. Frequent appointments in the days following repositioning ensure the flap is healing properly and vision is recovering as expected.
The success of treatment depends heavily on how quickly it is performed. When addressed within hours, flap repositioning typically restores clear vision with minimal long-term impact. Delayed treatment increases the risk of complications such as irregular astigmatism, scarring, or persistent visual distortion.
Prevention of Flap Dislocations
The vast majority of flap dislocations are preventable. Following your surgeon’s post-operative instructions carefully makes a significant difference:
- Do not rub your eyes. This is the single most important rule, particularly during the first three months. Wear the protective eye shield at night as directed to prevent unconscious rubbing while asleep.
- Avoid strenuous activities early on. Heavy lifting, intense bending, and exercises that increase head pressure should be paused for at least one week.
- Wear protective eyewear during sports. Even years after LASIK, sport-specific goggles or polycarbonate shields are a wise investment—especially for boxing, football, and racquet sports.
- Protect your eyes from debris and irritants. Be cautious around dust, wind, and smoke in the early weeks. Wraparound sunglasses offer practical protection outdoors.
- Attend every follow-up appointment. Your surgeon monitors flap adhesion, tear film health, and corneal healing at each visit. Skipping appointments means potential issues go undetected.
Knowledge Is Power for a Smooth LASIK Recovery
LASIK flap dislocation is genuinely rare—and with modern femtosecond technology and careful post-operative protocols, the risk is lower than ever. But understanding the condition empowers you to act fast if something feels wrong, and more importantly, to take the simple preventive steps that make complications unlikely in the first place.
At Visual Aids Centre, we walk every patient through detailed recovery guidelines during their pre-surgical consultation and provide rapid-access emergency support after surgery. If you are considering LASIK or have concerns about your recovery, book a consultation with our team and get answers specific to your eyes.
Frequently Asked Questions (FAQs)
How common is LASIK flap dislocation?
Flap dislocation occurs in fewer than 1–2% of cases during the early post-operative period. Late dislocations caused by trauma are even rarer. Proper aftercare dramatically reduces the risk.
Can a dislocated flap heal on its own?
No. A displaced flap requires professional repositioning by an ophthalmologist. Leaving it untreated can lead to irregular healing, infection, or permanent visual distortion.
How do I know if my LASIK flap has moved?
Sudden blurry vision, sharp pain, a foreign body sensation, or unusual light sensitivity are the key warning signs. If any of these appear, contact your surgeon immediately.
Can the flap be dislodged years after LASIK?
It is extremely rare but possible if the eye sustains significant blunt trauma. This is why protective eyewear during contact sports is recommended indefinitely after LASIK.
Is flap dislocation a risk with SMILE Pro surgery?
No. SMILE Pro is a flapless procedure that extracts a small lenticule through a tiny incision, so there is no flap to displace. It may be a better option for patients in high-contact professions or sports.
What happens if I accidentally poke my eye after LASIK?
Apply preservative-free lubricating drops and avoid touching the eye further. If you notice any vision changes, pain, or redness, see your surgeon promptly for evaluation.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Post-Operative Care Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With more than four decades of clinical experience and over 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey has refined every aspect of post-LASIK patient care—from surgical technique to the everyday recovery advice that prevents complications. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey personally reviews post-operative care protocols at the centre to ensure patients receive guidance grounded in real-world outcomes, not generic instructions. Learn more about our story and the team behind Visual Aids Centre.