If your ophthalmologist has just sealed a retinal tear with laser photocoagulation — or you’re scheduled for one soon — the procedure itself probably took less than 15 minutes. But what happens next? The recovery period after retinal laser surgery is straightforward for most patients, yet there are specific symptoms, timelines, and restrictions you need to understand to heal safely.
Retinal laser treatment is fundamentally different from refractive procedures like Femto LASIK or SMILE Pro. It doesn’t correct your glasses prescription — it prevents a tear from progressing into a full retinal detachment, which is a sight-threatening emergency. This guide covers exactly what to expect in the hours, days, and weeks following retinal laser surgery, what’s normal, what isn’t, and when to call your surgeon immediately.
Key Takeaways
- Retinal laser photocoagulation seals a tear by creating a controlled scar around it — not by repairing the tear itself.
- Blurry vision, light sensitivity, and mild headache for 24–48 hours are normal and expected.
- Avoid heavy lifting, straining, and jarring physical activity for 1–2 weeks to let the laser scar mature.
- New flashes of light, a sudden increase in floaters, or a curtain-like shadow in your vision after the procedure are emergency warning signs — contact your surgeon immediately.
What Is Retinal Laser Surgery and Why Is It Done?
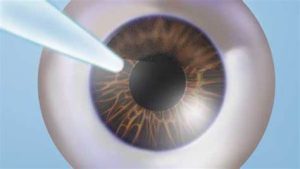
Retinal laser surgery — technically called laser photocoagulation or laser retinopexy — uses a focused laser beam to create tiny burns around a retinal tear or hole. These burns produce scar tissue as they heal, welding the retina to the underlying pigment epithelium and preventing fluid from seeping beneath the retina and causing a detachment.
The procedure is usually performed as an outpatient treatment. Your pupil is dilated, a contact lens is placed on the eye for focusing, and the surgeon delivers 50–200+ laser spots around the tear. The entire process takes 10–20 minutes. It’s preventive — the goal is to stop a tear from becoming something far more serious. Patients who are being evaluated for refractive surgery sometimes discover retinal tears during their pre-operative retinal examination, and these need to be treated and fully healed before proceeding with any corneal procedure.
What Happens Immediately After the Procedure
In-Clinic Recovery (First 30 Minutes)
Immediately after laser treatment, your vision will be noticeably blurry — this is primarily from the dilating drops, not the laser itself. The bright light from the laser may leave a temporary afterimage or a dull ache behind the eye. Most patients describe the sensation as a mild headache rather than sharp pain. You’ll rest in the clinic for 15–30 minutes while the clinical team checks that everything looks stable. No patch or shield is typically needed.
Getting Home Safely
Because your pupils are dilated and your vision is blurry, you cannot drive yourself home. Arrange for someone to accompany you — the same advice applies to patients recovering from any eye procedure requiring dilation. Bring sunglasses — your eyes will be extremely light-sensitive for several hours. Expect the dilation to last 4–6 hours; some patients remain light-sensitive into the next morning.
Day-by-Day Recovery Timeline
Day 1 — Blurry Vision, Light Sensitivity, Mild Discomfort
The day of the procedure is the most uncomfortable. Vision is blurred (partly from dilation, partly from mild retinal swelling around the laser spots). Light sensitivity can be significant — staying in a dimly lit room with soft, indirect lighting helps considerably. A dull ache or pressure sensation behind the eye is common and usually responds well to paracetamol. If your surgeon has prescribed anti-inflammatory drops, begin using them as directed.
Days 2–3 — Gradual Clearing
By the second day, most patients notice their vision beginning to clear. Light sensitivity decreases substantially. The aching sensation typically resolves. Some patients see a faint grid pattern or small dark spots in their peripheral vision where the laser spots were placed — this is normal and usually fades over the following weeks as the scars mature. Mild floaters may persist or even seem slightly more noticeable as the vitreous gel settles, but they shouldn’t increase dramatically.
Days 4–7 — Near-Normal Comfort
By the end of the first week, comfort levels are essentially back to normal for most patients. You can resume light daily activities, reading, and moderate screen use. Vision should be close to your pre-procedure baseline — retinal laser doesn’t change your prescription, so your glasses or contact lens power remains the same. Avoid strenuous exercise, heavy lifting, and anything that significantly increases pressure inside the eye during this period.
Weeks 2–4 — Follow-Up and Scar Formation
Your surgeon will schedule a follow-up examination (usually at 1–2 weeks and again at 4–6 weeks) to check that the laser scars have formed properly and the retinal tear is sealed. During this appointment, the retina is examined with a dilated fundus exam to ensure no new tears have developed. The adhesion created by the laser reaches full strength at approximately 2–3 weeks. Until your surgeon confirms the seal is secure, continue to follow activity restrictions.
Normal Symptoms vs Warning Signs
Understanding the difference between expected healing symptoms and signs of a complication is critical. Normal post-procedure symptoms include mild blurriness for 1–2 days, light sensitivity (photophobia) for 24–48 hours, dull ache behind the treated eye on day 1, small dark spots in peripheral vision where laser was applied, and pre-existing floaters that remain unchanged or improve slightly over weeks.
Emergency warning signs that require immediate contact with your surgeon include a sudden shower of new floaters (not pre-existing ones — a dramatic increase), new flashes of light that weren’t present before, a shadow or curtain effect creeping across any part of your visual field, a sudden significant drop in vision, or severe eye pain that doesn’t respond to over-the-counter painkillers. These symptoms could indicate that the tear has extended, a new tear has formed, or a retinal detachment is developing — all of which require urgent intervention. Don’t wait for your scheduled follow-up; call your clinic or go to an emergency eye department immediately. If you’ve experienced posterior vitreous detachment previously, you should be especially vigilant about these symptoms.
Activity Restrictions After Retinal Laser Surgery
The laser spots need time to form a strong adhesive scar. During the first 1–2 weeks, avoid activities that increase intraocular pressure or risk jarring the eye. Heavy lifting (anything requiring you to strain or hold your breath), bending with your head below your waist for extended periods, vigorous exercise, running, jumping, and contact sports are all off-limits in the early recovery window. Swimming should wait at least 2 weeks due to infection risk.
Light walking, desk work, cooking, and normal household tasks are generally fine from day 2 onward. Air travel is usually safe after retinal laser (unlike after some retinal detachment surgeries involving gas bubbles), but confirm with your surgeon before booking a flight. If you wear contact lenses, ask your doctor when it’s safe to reinsert them — most surgeons advise waiting a few days to a week. Patients with eye strain concerns from screens can manage with regular breaks and lubricating drops during recovery.
Will Your Vision Improve After the Procedure?
This is one of the most common misconceptions. Retinal laser surgery does not improve your vision — it preserves it. The purpose is to prevent a retinal tear from becoming a detachment, which would cause severe, potentially permanent vision loss. If the tear was in your peripheral retina (most are), you may not have noticed any vision change before or after treatment. If it was closer to the macula (the central vision area), you might have experienced distortion or a blind spot — the laser prevents this from getting worse, but it doesn’t reverse existing damage.
Patients who were experiencing flashes and floaters before the laser may notice that flashes reduce or stop once the vitreous traction stabilises. Floaters, however, tend to persist — they’re caused by vitreous changes, not by the tear itself, and laser treatment doesn’t address them. Over months, the brain often adapts and floaters become less noticeable. For patients who are also considering refractive surgery to reduce dependence on glasses, the retinal tear must be fully healed and confirmed stable (usually 4–6 weeks minimum) before any corneal procedure is performed. The importance of retinal assessment in the pre-operative process cannot be overstated.
How Retinal Laser Relates to LASIK and Other Eye Surgeries
If you’re reading this because a retinal tear was found during your pre-LASIK evaluation, here’s the typical sequence: the retinal tear is treated first with laser photocoagulation, followed by a waiting period of 4–6 weeks for the scar to mature, then a repeat retinal examination to confirm the seal is strong, and only then does the refractive surgery team proceed with your LASIK, Contoura Vision, or SMILE Pro procedure.
This is why comprehensive pre-operative testing matters. A retinal tear that goes undetected before refractive surgery could worsen during or after the procedure — particularly if the suction involved in flap creation stresses the vitreoretinal interface. At Visual Aids Centre, the pre-surgical evaluation includes a dilated fundus examination and, when indicated, advanced diagnostic imaging of the peripheral retina. Treating a tear before it becomes a detachment is infinitely simpler and safer than managing a detachment after it occurs. Patients with high myopia (above -6.00 dioptres) are at elevated risk for retinal tears — if this applies to you, our article on high-power LASIK eligibility discusses the additional screening steps involved.
The Bottom Line
Recovery after retinal laser surgery is typically quick and uncomplicated — most patients feel essentially normal within a week. The critical points: expect blurriness and light sensitivity for 1–2 days, avoid strenuous activity for 1–2 weeks, attend all follow-up appointments, and know the emergency warning signs (new flashes, sudden floater shower, shadow in vision). The laser doesn’t improve your sight — it protects it from a far worse outcome. If you’ve been told you need retinal laser treatment or you’re preparing for refractive surgery and want a thorough retinal evaluation first, book an appointment at Visual Aids Centre for a comprehensive assessment.
Frequently Asked Questions (FAQs)
How long does it take to recover from retinal laser surgery?
Most patients feel comfortable within 2–3 days and return to normal activities within a week. Full scar maturation takes 2–3 weeks, during which activity restrictions apply.
Is retinal laser surgery painful?
The procedure itself may cause a brief stinging or aching sensation with each laser pulse, but it’s tolerable for most patients. Post-procedure discomfort is typically a dull ache that resolves within 24 hours with simple painkillers.
Can I watch TV or use my phone after retinal laser?
Yes, light screen use is fine from day 1 — there’s no restriction on screens. However, your vision will be blurry from dilation for several hours, so you may not find it comfortable until the next day.
Will I need glasses after retinal laser surgery?
Retinal laser doesn’t change your glasses prescription. If you wore glasses before, you’ll continue to need the same prescription afterward. Refractive correction requires a separate procedure like LASIK or SMILE Pro.
Can a retinal tear come back after laser treatment?
The treated tear itself is sealed permanently by the laser scar. However, new tears can develop in a different area of the retina, especially in patients with high myopia or ongoing vitreous changes. Regular retinal check-ups are important.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Retinal Assessment Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
The recovery guidance in this article reflects clinical protocols used at Visual Aids Centre, where retinal assessment is an integral part of every pre-operative evaluation. Dr. Vipin Buckshey—an AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India—ensures that every patient undergoing refractive surgery receives a thorough dilated retinal examination, with any tears identified and treated before corneal procedures proceed.