Table of Contents
ToggleIntroduction
In brief, yes, eyelid surgery leaves scars, but these scars are nearly undetectable. The scars’ position is determined by the incisions used to execute the blepharoplasty procedure:
Upper eyelids: The natural crease usually makes incisions in the upper eyelid. Typically, the scars that occur are well hidden in the skin inside the folds.
Lower eyelids: In the lower lash line, Incisions are made which conceal them well. Suppose you’re having lower eyelid surgery with a “transconjunctival” method to remove pockets of extra fat underneath your eyes. In that case, an incision will be made on the inside of your lower eyelid, where no one can see it. The transconjunctival method eliminates fat and does not affect sagging skin.

Background
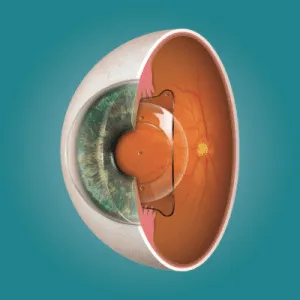
After epikeratoplasty, laser in situ keratomileuses have been described with satisfactory early results; however, no significant long-term follow-up has been documented. This case highlights the potential for corneal haze and scarring after LASIK within the epikeratoplasty lenticule generated by LASIK flap generation, excimer laser ablation, or both in the epikeratoplasty lenticule. Scarring necessitated full-thickness PKP in one eye for visual rehabilitation, and acuity in the unoperated eye remained limited.
Because epikeratoplasty was advertised as a reversible operation, few patients would require more than a simple lenticule excision if ametropia or other issues developed after the procedure. However, some histopathologic features have been observed in past cases after lenticule removal, including thickened epithelium, collagenous subepithelial fibrocelluar tissue, disrupted Bowman layer, scarred and edematous stroma, and keratocytes surrounding the Bowman layer. Electron microscopy revealed basement membrane abnormalities and duplications and a reduction in hemidesmosomes. Cases of corneal scarring in the recipient that did not improve after the graft was removed have also been documented. Rodrigues et al. report say that uneven collagen, focal posterior stromal fibrosis, persistent Descemet folds, and focal endothelial degeneration is in the host Bowman layer. In other cases, lenticular keratocytes, fibrogranular material, and recipient keratocyte migration into the lenticule have all been reduced.
It was discovered Bowman layer disturbance in both the lenticule and the host, as well as scarring. We found Bowman layer disruption in both the lenticule and the host and scarring at the host-lenticule contact. Keratocyte migration was seen using electron microscopy at the LASIK flap and lenticule junction. In a series of epikeratoplasty grafts, keratocyte migration from the periphery to the center of the lenticule was also observed. Due to steep keratometry readings, Lee and Manni describe using the keratome to create a buttonhole in an epikeratoplasty button. In multiple patients, Kim et al. describe lenticule separation following microkeratome in situ keratomileuses without suture, which was difficult to repair and resulted in epithelial ingrowth. Scarring of the donor or lenticule tissue may result from microkeratome damage. It is yet to be determined whether femtosecond LASIK with epikeratoplasty is safe and effective. There is the worry that a femtosecond laser could create an ultrathin flap, resulting in a postoperative haze, as shown with ultrathin flaps with a similar outcome to our patient. Targeting a thicker-than-usual flap with femtosecond LASIK may be a superior option As recipient keratocyte migration into the lenticule. However, in the case of LASIK after epikeratoplasty, migration has not been seen.
Discussion
In addition to scarring and keratocyte migration, performing LASIK after epikeratoplasty poses hazards. When a mechanical microkeratome is used over a lenticule, the lenticule may dislocate or be damaged.
If femtosecond LASIK is used, targeting a thicker-than-usual flap to avoid the lenticule may be a better option; however, as seen in the patient’s left eye, even a thick LASIK is used flap into the host stroma might result in visible scarring.
Surface ablation may be a better choice than LASIK for avoiding these concerns, and it can also be utilized to alleviate anterior scarring on the lenticule in some cases; nevertheless, haze has been documented in the literature following most PRK after epikeratoplasty circumstances.
Mitomycin-C (MMC) was not employed in these studies. However, its usage could reduce the production of haze. With a 6-month follow-up, a case study of ten patients showed improvement in astigmatism and visual acuity with topography-guided laser-assisted subepithelial keratectomy. 19 However, as demonstrated in our case, a longer follow-up is required to assess whether surface ablation is a good technique for epikeratoplasty patients.
Experience
If ulcers or injuries to the cornea penetrate beyond the layers of the epithelium, scars can occur. Because the cornea’s inner layers do not recycle like the outer epithelial layer, these scars will most likely be permanent. These superficial scars are usually not a concern for LASIK unless they are thick and deep, in which case they may interfere with the flap development.
PRK can eliminate these scars since it addresses both the underlying Bowman’s layers and the outer layers of the stroma, although it takes longer to heal than LASIK. Most surgeons will not change procedures to get rid of a scar that does not affect vision if the wounds are not obstructing vision performance.
Conclusion
LASIK following epikeratoplasty can cause corneal haze and scarring that necessitate corneal transplantation for visual rehabilitation. Even though epikeratoplasty is no longer performed, people with a history of the procedure may seek surgical alternatives to vision correction. If LASIK therapy is planned, we recommend exploring surface ablation treatments with MMC and avoiding the use of a mechanical microkeratome.