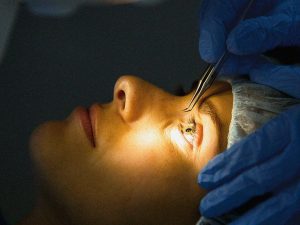
If your vision suddenly blurs, your eye starts hurting sharply, and light becomes unbearable in the days after LASIK—your corneal flap may have shifted. Flap dislocation is rare, but recognising the signs quickly is the difference between a straightforward fix and a serious complication.
During LASIK surgery, a thin flap is created on the corneal surface, lifted so a laser can reshape the tissue underneath, and then repositioned. In the first days and weeks, this flap is healing and reattaching—but it is not yet firmly bonded. A direct impact, vigorous eye rubbing, or even sleeping face-down on the pillow can potentially dislodge it. This guide walks you through the exact symptoms that distinguish a displaced flap from normal post-operative recovery, explains when the flap is most vulnerable, tells you precisely what to do if you suspect movement, and covers the prevention strategies that make dislocation extremely unlikely.
Key Takeaways
- A displaced LASIK flap causes a sudden, dramatic change—sharp pain, significant vision drop, intense light sensitivity, and excessive tearing—not the gradual mild blurriness of normal healing.
- The highest-risk window is the first 24–72 hours after surgery; risk decreases substantially after one week and is very low after three months.
- If you suspect flap movement, do not touch your eye—apply your protective shield and contact your surgeon immediately for same-day assessment.
- When caught early, a displaced flap can be repositioned with excellent visual outcomes in most cases.
What Is the LASIK Flap and Why Can It Move?
During LASIK, a femtosecond laser creates a thin hinged flap—typically 90–120 microns thick—on the front surface of the cornea. This flap is lifted to expose the stromal tissue underneath, which the excimer laser then reshapes to correct your refractive error. After reshaping, the flap is laid back into position, where it adheres through natural suction and begins healing without stitches.
In the first hours and days, the flap is held in place primarily by surface tension and the epithelial cells that begin bridging across the flap edge. There are no sutures anchoring it. This means that during the early healing window, sufficient force applied to the eye—whether from rubbing, a direct blow, or even strong pressure from sleeping position—can theoretically shift the flap from its correct alignment. Understanding the stages of flap healing helps you appreciate why the first few days demand such careful attention.
The Symptoms of a Displaced LASIK Flap
If your flap has shifted, the symptoms are typically sudden, unmistakable, and significantly different from normal post-operative discomfort. Here is what to watch for.
Sudden, Sharp Eye Pain
Normal LASIK recovery involves mild irritation—a gritty, scratchy sensation that settles within a few hours. A displaced flap causes a distinctly sharper, more intense pain that does not resolve with lubricating drops. If you experience a sudden spike in pain after a period of relative comfort—particularly following an incident like accidentally rubbing your eye or bumping your face—take it seriously.
Significant, Sudden Vision Drop
This is the most alarming symptom. Vision that was improving or stable suddenly becomes markedly blurry—not the mild haze of early recovery, but a dramatic decline that may make it difficult to read large text or recognise faces. The blurriness typically affects the operated eye specifically and does not improve with blinking or artificial tears.
Intense Light Sensitivity
A displaced flap disrupts the smooth corneal surface, scattering light irregularly. This causes sudden, severe light sensitivity that goes well beyond the mild photophobia most patients experience in the first day or two. Even indoor lighting may feel painfully bright, and you may instinctively want to keep the affected eye shut.
Excessive, Uncontrollable Tearing
The eye responds to the exposed stromal tissue and irregular surface by producing a flood of reflex tears. This tearing is typically more intense and persistent than the normal watery eyes experienced in early LASIK recovery.
Visible Irregularity or Foreign Body Sensation
Some patients describe a persistent feeling that something is “in” the eye—different from the mild scratchiness of normal healing. In some cases, the displaced flap edge may be visible as a subtle line or fold when looking closely in a mirror, though you should never attempt to examine or manipulate your eye yourself.
Normal Recovery vs. Flap Dislocation: How to Tell the Difference
This distinction is critical, because mild discomfort and blurry vision are completely expected in the first 24–48 hours after LASIK. The difference lies in the pattern and severity. Normal recovery involves mild grittiness that improves steadily, vision that is hazy initially but clears progressively over hours, moderate light sensitivity that is manageable with sunglasses, and mild tearing that settles by the end of day one.
Flap dislocation, by contrast, involves a sudden worsening after initial improvement (or after a specific incident), sharp pain rather than mild irritation, dramatic vision loss rather than gradual haze, and light sensitivity severe enough to prevent opening the eye. The key word is “sudden.” Normal recovery is a gradual trend toward improvement. Flap displacement is an abrupt deterioration—often clearly linked to a triggering event like bumping the eye, rubbing it, or removing the protective eye shield too early.
When Is the Flap Most Vulnerable?
First 24–72 Hours: Highest Risk
The flap has had minimal time to begin healing. Epithelial cells are just starting to bridge the flap edge. Any direct contact with the eye—even a seemingly gentle rub while half-asleep—can displace it during this window. This is why your surgeon prescribes protective shields, especially for sleeping.
Week 1–4: Moderate Risk
The epithelium has sealed across the flap edge, providing meaningful adhesion. However, the deeper stromal healing that ultimately anchors the flap is still incomplete. A forceful impact—an elbow during sports, a child’s hand hitting your face—could still dislodge the flap. Follow your surgeon’s restrictions on returning to sports and physical activities during this period.
Month 1–3: Low but Not Zero
By this stage, the flap is substantially adhered. Displacement from normal daily activities is extremely unlikely. However, significant blunt trauma to the eye could still theoretically cause issues, which is why protective eyewear remains advisable for contact sports indefinitely after LASIK.
Beyond 3 Months: Very Rare
Late flap dislocation is documented in medical literature but is exceptionally rare—typically requiring severe direct trauma to the eye. For most patients, the flap adhesion is effectively permanent by this point for all practical purposes.
What Causes the Flap to Shift?
The most common cause is eye rubbing in the early recovery period—often happening unconsciously during sleep, which is precisely why protective shields at night are non-negotiable. Direct trauma to the eye—a finger poke, a ball, an accidental knock—is the second most common cause. Some patients have experienced displacement after forcefully squeezing their eyes shut or from vigorous face washing too close to the eye area. Pre-existing conditions like severe dry eye can also compromise flap adhesion by affecting the epithelial healing process, and certain flap-related complications like striae (wrinkles) can make the flap more susceptible to displacement.
What to Do If You Suspect Your Flap Has Moved
If you experience the symptoms described above—especially a sudden combination of sharp pain, vision drop, and light sensitivity after a triggering event—take these steps immediately. First, do not touch, rub, press, or attempt to examine the eye. Any manipulation risks worsening the displacement. Second, place your protective eye shield over the affected eye if you have it available. Third, instil a drop of preservative-free artificial tears if you can do so without pressing on the eye—this keeps the surface moist. Fourth, contact your surgeon’s emergency line immediately. Most LASIK centres, including Visual Aids Centre, maintain same-day emergency access for post-operative patients. If your surgeon is unreachable, go to an eye hospital emergency department. Do not wait until the next scheduled follow-up—flap repositioning outcomes are best when addressed within hours, not days.
What Happens at the Clinic
Your surgeon will examine the eye under a slit lamp to confirm whether the flap has shifted and assess the degree of displacement. If the flap has moved, the standard treatment is repositioning—the surgeon lifts the flap, irrigates the interface to remove any debris or epithelial cells that may have migrated underneath, and carefully realigns the flap. This procedure is typically performed under topical anaesthesia and takes only a few minutes. After repositioning, you will be placed back on antibiotic and anti-inflammatory drops, and the protective shield protocol restarts. For a deeper understanding of this process, see our article on LASIK flap repositioning. When caught promptly, visual outcomes after repositioning are typically excellent—most patients recover the same quality of vision they had before the displacement occurred.
How to Prevent Flap Displacement
Prevention is straightforward and comes down to following your post-operative instructions closely. Wear protective eye shields while sleeping for the full duration your surgeon recommends—typically one to two weeks. Do not rub your eyes for at least four weeks, and be gentle with the eye area for several months. Avoid contact sports, swimming, and activities with a risk of eye impact for the time frame your surgeon specifies. When washing your face, keep water and pressure away from the eyes—use a damp cloth rather than splashing. Attend every scheduled follow-up appointment so your surgeon can confirm the flap is healing properly and catch any early signs of complications before they become problems.
Conclusion
A displaced LASIK flap announces itself unmistakably: sudden sharp pain, dramatic vision loss, severe light sensitivity, and excessive tearing—usually following a specific triggering event. If your recovery is a steady, gradual improvement with mild discomfort, your flap is almost certainly fine. But if you experience an abrupt deterioration—especially in the first week—do not wait, do not self-diagnose, and do not touch your eye. Contact your surgeon immediately. When treated promptly, flap repositioning has excellent outcomes and your vision can be fully restored. If you are considering LASIK and want to understand the full recovery process and safety protocols, book a consultation at Visual Aids Centre for a personalised assessment.
Frequently Asked Questions (FAQs)
Can a LASIK flap move years after surgery?
It is extremely rare but documented in cases of severe direct trauma to the eye. After three months, the flap adhesion is strong enough that normal daily activities pose virtually no risk of displacement.
How do I tell if my blurry vision is normal or a flap problem?
Normal post-LASIK blurriness is mild, present from the start, and improves gradually. A flap issue causes a sudden, dramatic vision drop—often after a specific incident like rubbing the eye or a bump—following a period of improvement.
Can I check if my flap moved by looking in a mirror?
Do not attempt to self-examine. The flap is nearly invisible to the naked eye, and touching or manipulating the eye can worsen any displacement. Let your surgeon examine you with a slit lamp.
What happens if a displaced flap is not treated quickly?
Delayed treatment increases the risk of epithelial ingrowth (cells growing under the flap), infection, irregular healing, and permanent vision impairment. Same-day assessment is strongly recommended.
Does SMILE surgery have the same flap displacement risk?
No. SMILE is a flapless procedure—it uses a small lenticule extraction incision rather than creating a full corneal flap, so flap dislocation is not a risk. This is one reason some patients and surgeons prefer SMILE for those with active lifestyles or contact-sport involvement.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Post-Operative Care Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With over four decades of clinical experience and more than 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey has managed every category of post-LASIK complication—including flap displacement—across a career spanning the full evolution of refractive surgery technology. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey personally oversees post-operative protocols at the centre to minimise complication risk and ensure rapid intervention when needed.