You’ve been told your cornea is too thin for LASIK. It’s one of the most frustrating things a patient can hear—especially after building up the courage to finally ditch glasses. But a thin cornea doesn’t necessarily mean laser vision correction is off the table. In many cases, SMILE (Small Incision Lenticule Extraction) or its advanced version SMILE Pro may be exactly the procedure that works where LASIK cannot.
The reason comes down to biomechanics. SMILE removes tissue from within the cornea through a tiny keyhole incision—no flap required. This single difference preserves significantly more corneal structural strength than LASIK, making it a viable option for patients whose corneal thickness falls below the LASIK safety threshold. This guide from Visual Aids Centre explains how thin your cornea can be for SMILE, why tissue conservation matters so much, and what to do if even SMILE isn’t feasible for your anatomy.
Key Takeaways
- SMILE preserves the anterior corneal stroma and Bowman’s layer—the strongest structural components—because it doesn’t create a flap.
- Patients with corneal thickness as low as 475–480 microns may qualify for SMILE, compared to the 500+ micron minimum typically required for LASIK.
- The critical number isn’t total corneal thickness alone—it’s the residual stromal bed (RSB) after tissue removal, which must stay above 250 microns.
- SMILE Pro (VisuMax 800) completes the lenticule creation in approximately 10 seconds, further reducing suction time and tissue stress.
What Counts as a Thin Cornea?
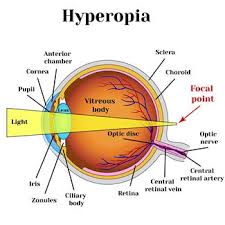
The average human cornea is about 540–550 microns thick at its centre. In refractive surgery, a cornea below 500 microns is generally considered thin, and anything below 480 microns is notably thin. Corneal thickness is measured using pachymetry—either ultrasound-based or optical (Pentacam/Orbscan)—and it’s one of the first numbers your surgeon checks during a pre-operative evaluation.
Why does this matter? Every laser vision correction procedure removes corneal tissue to reshape the eye’s focusing surface. The thinner your starting cornea, the less tissue is available to work with—and the higher the risk of weakening the cornea to the point where it bulges outward post-surgery, a condition called ectasia. Understanding what happens when the cornea is too thin for LASIK gives important context for why SMILE becomes the preferred option.
Why LASIK Isn’t Safe for Thin Corneas
In LASIK, a femtosecond laser creates a hinged flap—typically 100–120 microns thick—on the front surface of the cornea. The flap is lifted, the excimer laser reshapes the underlying stroma, and the flap is repositioned. The problem for thin-cornea patients is twofold.
First, the flap itself consumes 100–120 microns of thickness before any correction even begins. Second, the flap severs the anterior stromal fibres and Bowman’s layer—the cornea’s strongest structural components. Once these are cut, they never fully regain their original tensile strength. For a cornea that’s already on the thin side, this combination dramatically increases the risk of post-LASIK ectasia. This is precisely why surgeons turn to flapless alternatives for thin-cornea patients.
How SMILE Preserves More Corneal Tissue
SMILE takes a fundamentally different approach. Instead of creating a flap, the femtosecond laser creates a thin disc of tissue (called a lenticule) within the cornea’s interior, then the surgeon extracts it through a small 2–4 mm incision. No flap. No Bowman’s layer disruption across the corneal surface. The anterior stromal lamellae—which provide the majority of the cornea’s biomechanical strength—remain largely intact.
The practical result: SMILE leaves a stronger cornea after surgery compared to LASIK at the same prescription correction. Research consistently shows that corneal biomechanics are better preserved with SMILE than with flap-based procedures. For patients starting with 490 microns of corneal thickness, this difference can mean the gap between qualifying for safe treatment and being turned away entirely. You can see a broader comparison of approaches at LASIK vs SMILE vs Contoura vs SMILE Pro.
Minimum Corneal Thickness for SMILE
There isn’t a single universal cutoff—it depends on your prescription, because higher prescriptions require more tissue removal. However, most surgeons consider 475–480 microns as the lower practical limit for SMILE, provided the residual stromal bed stays safely above 250 microns after lenticule extraction.
Compare this to LASIK, where the effective minimum is closer to 500–510 microns for the same prescription. The 20–30 micron difference may sound trivial, but in corneal surgery, every micron counts. That margin can be the difference between eligibility and rejection. For a detailed look at how thickness calculations work, see how residual corneal thickness is calculated. The same RSB principles apply to SMILE—the surgeon just starts with more available tissue because there’s no flap consuming the first 100+ microns.
SMILE Pro: Even Better for Borderline Corneas
The SMILE Pro platform (Zeiss VisuMax 800) is the latest evolution of lenticule extraction technology. For thin-cornea patients specifically, it offers several advantages over the original SMILE platform.
Faster Laser Application
SMILE Pro creates the lenticule in approximately 10 seconds—compared to about 25 seconds with the original VisuMax 500. The shorter laser time means less suction duration on the eye, which reduces the transient IOP spike during the procedure. For corneas that are already structurally borderline, minimising mechanical stress during surgery is a meaningful safety benefit.
Smaller Incision
SMILE Pro uses a 2 mm incision versus the 3–4 mm incision in earlier SMILE versions. A smaller incision means even fewer anterior stromal fibres are severed, further preserving corneal strength. This is especially relevant for thin-cornea patients where every structural advantage matters.
Enhanced Centration
The VisuMax 800 offers improved cyclotorsion compensation and centration tracking, which means the lenticule is positioned more precisely within the stroma. Precise positioning ensures tissue is removed only where it’s needed, avoiding unnecessary thinning in peripheral zones. Understanding how much corneal tissue SMILE Pro actually removes helps put the efficiency of this approach in perspective.
Understanding the Residual Stromal Bed (RSB)
The residual stromal bed is the amount of untouched corneal tissue remaining beneath the area of treatment after surgery. It’s the single most important safety metric in any corneal refractive procedure—more important than total corneal thickness alone.
For LASIK, the RSB is calculated as: total corneal thickness minus the flap thickness minus the ablation depth. For SMILE, it’s simpler: total corneal thickness minus the cap thickness minus the lenticule thickness. Because the SMILE “cap” stays attached (it’s not a free flap), it continues to contribute to the cornea’s overall structural integrity—unlike a LASIK flap, which provides minimal biomechanical contribution after being cut and repositioned.
The minimum safe RSB is generally accepted as 250 microns, though many surgeons prefer 280–300 microns as an added safety margin. At Visual Aids Centre, we use Pentacam tomography to map corneal thickness across its entire surface—not just the centre—because the thinnest point (which may be paracentral) is what determines true surgical safety.
What If Your Cornea Is Too Thin Even for SMILE?
For patients whose corneal thickness or prescription makes even SMILE unsafe, there are still excellent options available.
TransPRK (Surface Ablation)
TransPRK is a no-touch, no-flap surface procedure that removes zero stromal tissue for structural creation—no flap, no cap. The entire available depth goes toward the optical correction. Recovery is slower (1–2 weeks for functional vision versus 1–2 days with SMILE), but it can treat patients whose corneas are too thin for any intrastromal procedure.
ICL (Implantable Collamer Lens)
For patients with very thin corneas and high prescriptions, an implantable collamer lens (ICL) bypasses the cornea entirely. A biocompatible lens is placed behind the iris and in front of the natural lens, correcting vision without removing any corneal tissue at all. It’s fully reversible and particularly well-suited for prescriptions beyond -8 dioptres where corneal procedures would require too much tissue removal regardless of corneal thickness.
C3R + SMILE (Combined Approach)
In select borderline cases, some surgeons perform corneal collagen cross-linking (C3R) either before or simultaneously with SMILE to strengthen the corneal stroma and reduce the risk of post-operative ectasia. This combined approach is still emerging but shows promise for patients who fall just outside standard SMILE eligibility. Learn more about cross-linking at our C3R eye surgery page.
How the Pre-Operative Evaluation Works
Determining whether your thin cornea qualifies for SMILE requires far more than a single pachymetry reading. At Visual Aids Centre, the evaluation includes corneal tomography (Pentacam) to map thickness from edge to edge, corneal topography to screen for early keratoconus or irregular patterns, wavefront aberrometry to plan the precise lenticule profile, and a thorough review of your prescription history to confirm prescription stability.
The surgeon then calculates the exact RSB based on your thinnest corneal point—not the average—and determines whether SMILE, SMILE Pro, TransPRK, or ICL is the safest route. If you’ve been told your cornea is too thin for LASIK and want to know if SMILE is an option, book a comprehensive evaluation at Visual Aids Centre to get a definitive answer based on your specific measurements.
Conclusion
A thin cornea disqualifies you from LASIK in most cases—but not from laser vision correction altogether. SMILE and SMILE Pro preserve significantly more corneal tissue and structural integrity by eliminating the flap, making them viable options for many patients with corneal thickness in the 475–500 micron range. For corneas that are too thin even for SMILE, TransPRK and ICL provide excellent alternatives. The right answer always comes down to a thorough evaluation—your specific thickness, prescription, and corneal topography determine which procedure is safest and most effective.
Frequently Asked Questions (FAQs)
Can I get SMILE with a 480-micron cornea?
Potentially, yes—if your prescription is moderate and the residual stromal bed stays above 250 microns after lenticule extraction. Your surgeon must calculate this precisely using tomography data from your thinnest corneal point.
Is SMILE safer than LASIK for thin corneas?
Yes. SMILE preserves the anterior stroma and Bowman’s layer because it doesn’t create a flap. This results in a biomechanically stronger cornea after surgery, reducing the risk of ectasia—the primary concern with thin corneas.
What is the minimum corneal thickness for SMILE Pro?
There is no absolute minimum—it depends on your prescription. However, most surgeons consider 475–480 microns as the practical lower limit for SMILE Pro, provided the RSB calculation is within safe parameters.
What happens if my cornea is too thin for SMILE?
TransPRK (surface ablation) or ICL (implantable lens) are the primary alternatives. TransPRK avoids creating any cap or flap, while ICL bypasses the cornea entirely—ideal for very thin corneas with high prescriptions.
Does SMILE remove less corneal tissue than LASIK?
For the same prescription, the actual amount of tissue corrected is similar. However, SMILE doesn’t waste 100–120 microns creating a flap, so the net corneal tissue preserved is significantly greater—which is precisely why thin-cornea patients can qualify for SMILE but not LASIK.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Vision Correction Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
The clinical protocols described in this article reflect the evaluation and treatment standards followed at Visual Aids Centre under the direct supervision of Dr. Vipin Buckshey. With over four decades of practice and more than 250,000 laser vision correction procedures supervised, Dr. Buckshey has extensive experience evaluating thin-cornea patients and determining the safest procedure for each individual’s anatomy.
An AIIMS alumnus, former President of the Indian Optometric Association, official optometrist to the President of India, and Padma Shri recipient, Dr. Buckshey personally reviews every thin-cornea case—assessing Pentacam tomography, residual stromal bed calculations, and corneal biomechanical indices—to ensure that the recommended procedure maximises both visual outcome and long-term corneal safety.