LASIK is one of the most effective treatments for astigmatism — but “effective” does not always mean “permanent in every single case.” If you are considering laser vision correction for astigmatism, or you have already had it and noticed subtle changes in your vision, the question is understandable: can astigmatism actually come back after LASIK?
The honest answer is yes, it is possible — but it is uncommon, and when it does happen, it is usually mild and manageable. Research suggests that fewer than 5% of LASIK patients experience meaningful astigmatism regression. This guide explains why it can recur, what factors increase the risk, how to recognise the early signs, and what your options are if it does happen. Whether you are in the planning stage or years post-surgery, this information will help you make confident decisions about your vision.
Key Takeaways
- Astigmatism can return after LASIK, but it affects fewer than 5% of patients — and is usually mild.
- The most common cause is corneal regression, where the tissue gradually shifts back toward its original shape.
- Higher pre-operative astigmatism, thin corneas, and age-related lens changes increase the risk of recurrence.
- If astigmatism does return, options include enhancement surgery, topography-guided treatments, or updated glasses or contacts.
How LASIK Corrects Astigmatism in the First Place
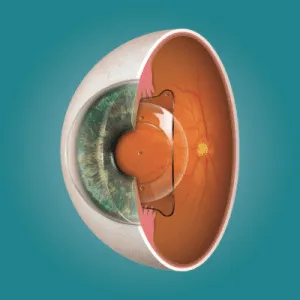
Astigmatism occurs when the cornea (or sometimes the lens) has an irregular curvature — shaped more like a rugby ball than a football. This uneven surface causes light to focus at multiple points instead of a single point on the retina, resulting in blurred or distorted vision at all distances.
During LASIK, an excimer laser precisely removes microscopic amounts of corneal tissue to reshape the surface into a more symmetrical curve. In procedures like Contoura Vision, the laser treatment is guided by a detailed topographic map of your individual cornea, allowing it to correct not just the overall cylinder but also subtle surface irregularities. Femto LASIK and SMILE Pro achieve similar goals through different techniques. The result, for most patients, is a cornea that focuses light cleanly — and astigmatism that is fully corrected.
Can Astigmatism Really Come Back?
Yes — but context matters. When eye surgeons say astigmatism “comes back,” they usually mean one of two things. The first is true regression, where the cornea gradually shifts back toward its pre-surgical shape over months or years. The second is new astigmatism caused by a different mechanism entirely, such as age-related changes in the crystalline lens inside the eye (lenticular astigmatism), which LASIK cannot prevent because it only reshapes the cornea.
The likelihood of clinically significant regression is low. Most studies place the rate at under 5%, and when it does occur, the returning astigmatism is typically milder than the original. A patient who had 3.00 dioptres of cylinder corrected might, for example, develop 0.50 to 0.75 dioptres of residual astigmatism — noticeable in certain lighting but far less debilitating than before surgery. For a deeper look at whether your vision can shift after surgery, see our article on whether your eyes can go bad again after LASIK.
Why Does Astigmatism Recur After LASIK?
Corneal Regression
The cornea is living tissue, and it heals. In some patients, the healing response causes the corneal surface to gradually remodel back toward its original curvature. This is more common when the initial correction was large — correcting 4.00 dioptres of astigmatism involves removing more tissue than correcting 1.00 dioptre, and the greater the change, the stronger the biological drive to “undo” it.
Epithelial Remodelling
The thin outer layer of the cornea (the epithelium) can thicken unevenly after surgery, subtly altering the refractive surface. This is different from stromal regression and is one reason corneal topography mapping at follow-up visits is so valuable — it can detect epithelial changes before you even notice symptoms.
Lenticular Changes with Age
As you age, the natural lens inside the eye can develop its own astigmatism, independent of whatever the cornea is doing. This lenticular astigmatism was not present when you had LASIK, so the surgery could not have corrected it. It is a new development, not a failure of the original procedure.
Incomplete Initial Correction
In a small number of cases, the laser may slightly undercorrect or overcorrect the astigmatism. This is not the same as regression — it is a residual error from the outset, typically identified at early follow-up visits. Our guide on LASIK enhancements for under- and over-correction explains how these situations are managed.
Who Is at Higher Risk of Regression?
Not every LASIK patient faces the same odds. Several factors can increase the likelihood that astigmatism returns after surgery.
High pre-operative astigmatism. Patients correcting more than 3.00 dioptres of cylinder have a statistically higher regression rate than those correcting 1.00 dioptre or less. The larger the correction, the more the cornea has to remodel, and the greater the chance of partial reversion. For patients with very high cylindrical power, understanding how cylindrical power is managed is useful.
Thin corneas. A thinner cornea means less stromal tissue is available as a buffer. If the residual stromal bed after surgery is on the thinner side, the biomechanical response can be less predictable. This is one reason thorough pre-LASIK testing is essential — it helps surgeons determine whether your cornea can safely support the intended correction long-term.
Younger age at surgery. Patients in their early 20s may still experience subtle prescription changes as their eyes finish maturing. Having a stable prescription for at least 12 months before LASIK is the standard safeguard against this.
Keratoconus or corneal weakness. If there is any underlying corneal instability, regression is far more likely — and in fact, standard LASIK may not be recommended at all. Conditions like keratoconus require different approaches such as C3R corneal cross-linking.
Warning Signs That Astigmatism May Be Returning
Astigmatism regression tends to develop gradually rather than overnight. Watch for blurred vision that seems to come and go — particularly at night or under low-contrast conditions — as well as difficulty reading small text, eye strain or headaches during prolonged screen work, and a sense that your vision “is not as sharp as it was a year ago.” If you experience any of these symptoms, schedule a check-up rather than waiting for your next routine visit. For more on recognising post-LASIK visual changes, our article on irregular astigmatism after LASIK provides additional detail.
What to Do If Astigmatism Comes Back
LASIK Enhancement (Touch-Up Surgery)
If you have sufficient corneal thickness remaining, a LASIK enhancement can re-lift the original flap and apply a second, smaller laser correction. This is the most common solution and is highly effective for mild regression. Learn more about how often enhancements are needed.
Topography-Guided Retreatment
For patients with irregular astigmatism — where the returning cylinder is not uniform — a topography-guided retreatment can map and correct the specific irregularities with higher precision than a standard retreatment.
Glasses or Contact Lenses
If the returning astigmatism is very mild (0.50 dioptres or less), some patients simply choose to manage it with part-time glasses for specific tasks like night driving. This is a perfectly valid choice and does not indicate a “failure” of the original procedure.
Alternative Procedures
In cases where the cornea is too thin for retreatment, options like PRK (surface ablation) or implantable lenses may be considered. Your surgeon will guide you toward the safest option based on your corneal thickness and overall eye health.
How to Minimise the Risk of Regression
Choose the right procedure and surgeon. Advanced platforms with cyclotorsion tracking and topography guidance are proven to deliver more precise astigmatism correction. At Visual Aids Centre, we use Contoura Vision, Femto LASIK, and SMILE Pro — selecting the best option for each patient’s specific corneal anatomy.
Wait for prescription stability. Do not rush into surgery if your prescription is still changing. A stable refraction for at least one year is the minimum benchmark.
Follow your post-operative care plan. Using prescribed drops on schedule, attending every follow-up appointment, and avoiding eye rubbing during healing all contribute to a stable corneal outcome.
Attend annual eye exams. Even years after LASIK, annual check-ups allow your surgeon to detect subtle changes early — before they become symptomatic — and recommend intervention if needed.
Conclusion
Astigmatism can come back after LASIK, but it is uncommon, usually mild, and almost always treatable. The key factors are the severity of your original astigmatism, the health and thickness of your cornea, the precision of the surgical platform, and how closely you follow post-operative care. For the vast majority of patients, LASIK delivers lasting astigmatism correction that holds up for decades. If you want to know whether your astigmatism is a good candidate for permanent correction, book a consultation at Visual Aids Centre — our pre-operative screening will give you a clear, personalised assessment of your expected outcomes and long-term stability.
Frequently Asked Questions (FAQs)
How common is it for astigmatism to return after LASIK?
Fewer than 5% of LASIK patients experience clinically significant astigmatism regression. When it does occur, the returning cylinder is usually much milder than the original.
How soon after LASIK can astigmatism come back?
Most regression happens within the first 6–12 months as the cornea heals and stabilises. Astigmatism returning years later is more often due to age-related lens changes rather than corneal regression.
Can a LASIK touch-up fix returning astigmatism?
Yes. If you have enough residual corneal thickness, a LASIK enhancement can re-correct mild astigmatism regression with high success rates.
Does Contoura Vision reduce the risk of astigmatism recurrence?
Topography-guided treatments like Contoura Vision correct corneal irregularities with greater precision, which may contribute to more stable long-term outcomes compared to standard LASIK for astigmatism.
Can astigmatism return if I rub my eyes after LASIK?
Chronic eye rubbing can weaken the cornea over time and potentially contribute to shape changes. Avoiding habitual rubbing is one of the simplest ways to protect your LASIK results.
Is SMILE Pro better than LASIK for treating astigmatism?
Both are effective for astigmatism correction. SMILE Pro preserves more corneal biomechanical strength because it does not create a flap, which may be an advantage for patients at higher risk of regression. Your surgeon will recommend the best option based on your specific profile.
👁️ MEDICALLY REVIEWED BY
Padmashree Dr. Vipin Buckshey
Optometrist & Post-Operative Care Specialist | AIIMS Graduate, 1977 | Padma Shri Honouree
With more than four decades of clinical experience and over 250,000 laser vision correction procedures performed at Visual Aids Centre, Dr. Vipin Buckshey has extensive experience managing astigmatism correction across all LASIK platforms — including complex cases involving high cylinder, irregular corneas, and post-surgical regression. An AIIMS alumnus, former President of the Indian Optometric Association, and official optometrist to the President of India, Dr. Buckshey personally oversees pre-operative screening protocols to identify regression risk factors before surgery, not after. Learn more about our team and legacy.